Introduction
If you are working with patients who complain of fatigue, non restorative sleep, or persistent metabolic dysfunction, there is a question worth asking more often in clinical practice. Are we looking at a sleep disorder, or are we looking at a state of chronic inflammation that is silently reshaping how sleep itself is structured?
Many practitioners are trained to evaluate sleep in terms of duration or symptoms. However, what often gets missed is sleep architecture, the internal organization of sleep stages that determines whether sleep is truly restorative. This is where inflammation begins to play a far more powerful role than most clinicians anticipate.
You may have seen this in practice. A patient sleeps for seven to eight hours but still wakes up exhausted. Another reports frequent awakenings without a clear mechanical cause. In many of these cases, the underlying issue is not just poor sleep hygiene. It is an altered neuro immune environment where inflammatory signaling is actively disrupting sleep regulation.
Understanding how chronic inflammation alters sleep architecture can change how you approach not only sleep disorders but also metabolic diseases, fatigue syndromes, and recovery physiology.
Sleep Architecture Is a Neuro Immune Process
What Defines Healthy Sleep Architecture
Sleep is not a passive state. It is a highly regulated biological process organized into cycles of non REM and REM sleep. Each stage has a distinct physiological role. Deep sleep supports physical repair, immune regulation, and hormonal balance. REM sleep is essential for cognitive processing and emotional regulation.
These stages are coordinated by complex interactions between the brain, endocrine system, and immune signaling molecules.
The Role of Cytokines in Sleep Regulation
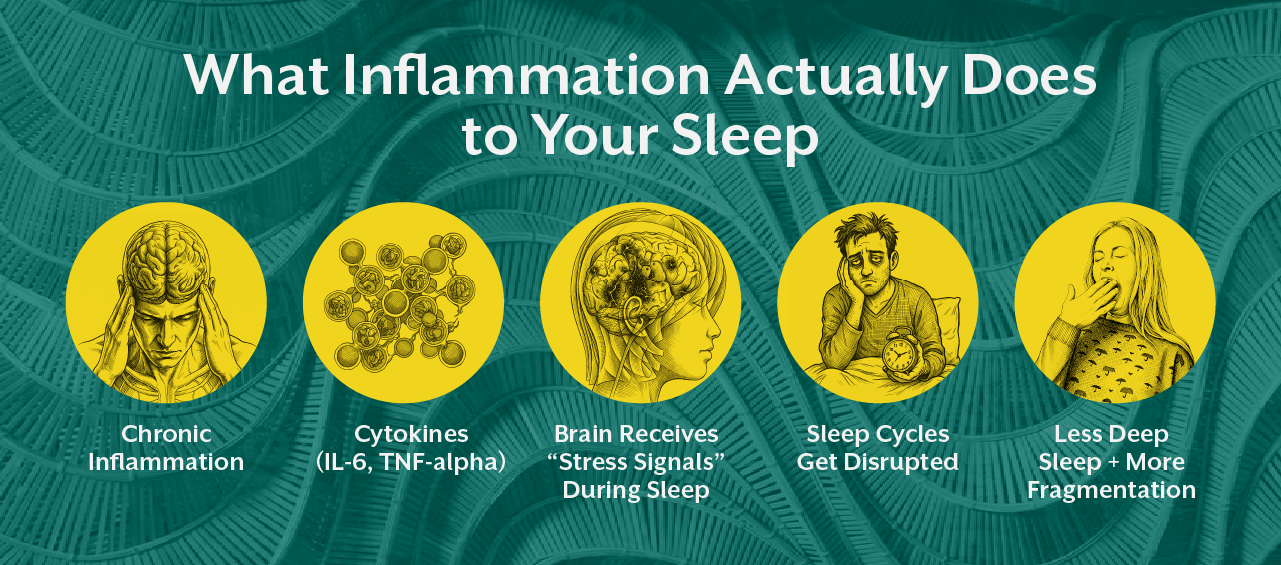
Cytokines are often discussed in the context of inflammation, but they also play a direct role in sleep physiology. Pro inflammatory cytokines such as interleukin six and tumor necrosis factor alpha influence sleep onset and depth. In acute conditions, this can be beneficial. For example, during infection, increased cytokine activity promotes sleep to support recovery.
However, when inflammation becomes chronic, this regulatory system becomes dysregulated. Instead of supporting sleep, cytokines begin to fragment it. Deep sleep duration reduces, REM cycles become unstable, and overall sleep quality declines.
When Inflammation Becomes Disruptive
Chronic inflammation does not simply increase or decrease sleep. It alters its architecture. Patients may experience lighter sleep, frequent awakenings, and reduced restorative phases even if total sleep time appears normal.
This is where the question “does inflammation affect sleep” becomes clinically significant. The answer is not only yes, but also that inflammation reshapes how sleep is structured at a fundamental level.
The Inflammation Sleep Feedback Loop
How Poor Sleep Fuels Inflammation
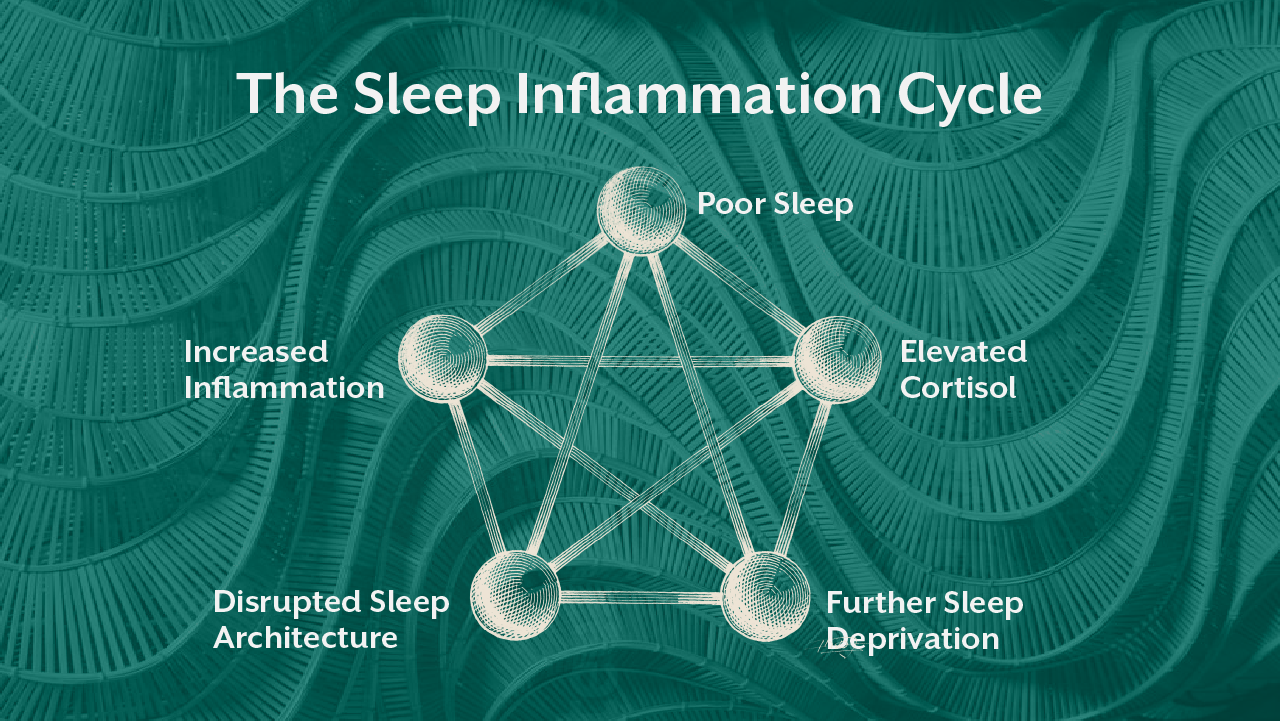
One of the most clinically relevant insights is that the relationship between inflammation and sleep is bidirectional. Sleep deprivation itself acts as a physiological stressor that increases inflammatory markers such as C reactive protein and interleukin six.
This means poor sleep causes inflammation, and inflammation further disrupts sleep. Over time, this creates a self sustaining cycle that is difficult to break without targeted intervention.
Cortisol and Inflammatory Signaling
Cortisol plays a central role in this interaction. Under normal conditions, cortisol follows a circadian rhythm, rising in the morning and declining at night. Chronic inflammation disrupts this rhythm. Elevated evening cortisol levels can prevent the transition into deep sleep, while blunted morning cortisol can reduce energy levels.
This dysregulation further contributes to poor sleep quality and metabolic dysfunction.
Clinical Relevance for Practitioners
If you are evaluating patients with chronic fatigue, metabolic syndrome, or persistent insomnia, it becomes essential to assess both sleep quality and inflammatory status. Looking at CRP levels and sleep patterns together often reveals patterns that would otherwise be missed.
For deeper understanding of how metabolic dysfunction develops in parallel with these changes, you may refer to the iThrive Academy blog “Metabolic Syndrome Explained: The Hidden Drivers of Chronic Disease” It provides a strong foundation for understanding systemic inflammation.
Mitochondrial Stress and Sleep Disruption
Energy Deficiency in the Brain
Sleep regulation requires energy. Neurons in the hypothalamus and brainstem depend on mitochondrial ATP production to maintain stable signaling. Chronic inflammation increases oxidative stress, which directly impairs mitochondrial function.
When mitochondrial efficiency declines, neuronal signaling involved in sleep regulation becomes unstable. This contributes to fragmented sleep and reduced sleep depth.
Oxidative Stress and Neural Signaling
Reactive oxygen species generated during chronic inflammation damage cellular structures, including mitochondrial DNA. This disrupts energy production and increases fatigue.
Patients often report feeling tired despite adequate sleep duration. This is not simply a sleep issue. It reflects underlying mitochondrial dysfunction.
For a deeper dive into this connection, the iThrive’s white paper on mitochondrial dysfunction and sleep deprivation provides valuable insights into how cellular energy impacts sleep disorders.
Nervous System Dysregulation in Chronic Inflammation
Sympathetic Dominance and Sleep Fragmentation
Chronic inflammation is closely linked with autonomic nervous system imbalance. Elevated inflammatory signaling increases sympathetic activity, keeping the body in a constant state of alertness.
This prevents the transition into deep parasympathetic states required for restorative sleep.
Why Patients Cannot “Switch Off”
Many patients describe an inability to relax at night. This is often interpreted as stress or anxiety, but from a physiological perspective, it reflects an inability of the nervous system to downregulate.
Repeated activation of stress pathways disrupts sleep architecture, leading to frequent awakenings and reduced sleep efficiency.
Connecting to Clinical Practice
If you are working with patients who report poor sleep despite lifestyle interventions, consider whether nervous system regulation is being adequately addressed. Breathwork, circadian alignment, and targeted nutrition can all support autonomic balance.
This concept is also explored in the iThrive Academy blog “Decoding Functional Sports Nutrition: How Electrolytes and HRV Define True Athletic Recovery,” where nervous system balance plays a key role in recovery physiology.
Why Practitioners Must Rethink Sleep Disorders
Beyond Symptom Based Diagnosis
Traditional approaches to sleep disorders often focus on symptoms such as insomnia or sleep apnea. While these diagnoses are important, they may not fully capture the underlying physiology.
Chronic inflammation alters sleep architecture at multiple levels including neuro immune signaling, hormonal balance, and mitochondrial function.
Integrating Functional Nutrition
Functional nutrition offers a framework to address these underlying mechanisms. By reducing inflammation, supporting mitochondrial health, and restoring circadian rhythm, practitioners can improve sleep quality at a foundational level.
Programs such as the iThrive Certified Functional Nutrition program are designed to help practitioners understand these connections and apply them in clinical practice.

Key Takeaway
Chronic inflammation is not just a contributing factor to poor sleep. It is a central regulator that reshapes sleep architecture at multiple levels. Through cytokine signaling, cortisol disruption, mitochondrial dysfunction, and autonomic imbalance, inflammation alters how the body enters, maintains, and benefits from sleep. For practitioners, this means that addressing sleep disorders requires more than improving sleep habits or prescribing mechanical interventions. It requires a deeper understanding of the inflammatory and metabolic environment influencing sleep physiology. By integrating functional nutrition, circadian biology, and nervous system regulation, clinicians can move beyond symptom management and support true recovery. This shift in perspective not only improves patient outcomes but also enhances the practitioner’s ability to address complex chronic conditions with greater precision.










.jpg)











