Introduction
For many practitioners entering metabolic or functional medicine practice, erectile dysfunction is often approached primarily as a hormonal or urological issue. Testosterone replacement, phosphodiesterase inhibitors, and psychological counseling frequently dominate the clinical discussion. Yet when viewed through a cardiometabolic lens, erectile dysfunction tells a much deeper story about systemic physiology.
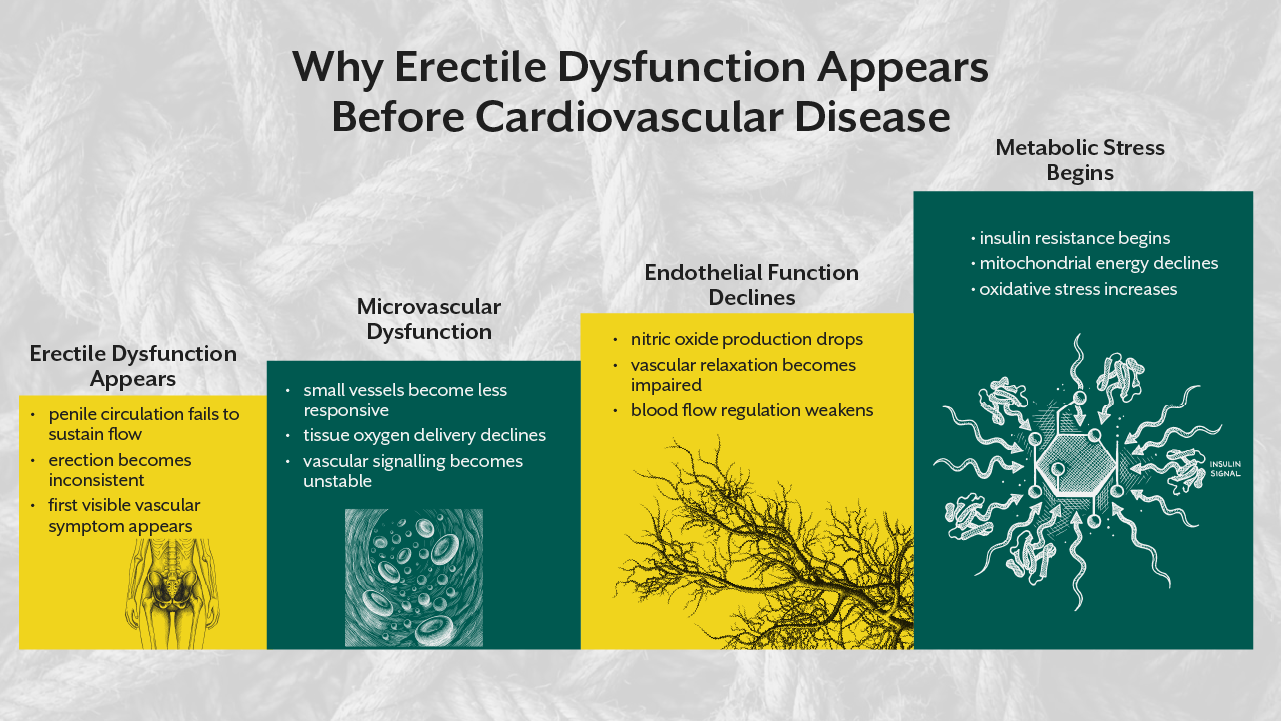
Erectile dysfunction is often the first visible sign of vascular dysfunction, insulin resistance, and autonomic imbalance that has been developing silently for years. In fact, emerging evidence suggests that erectile dysfunction can precede cardiovascular disease by several years, sometimes appearing before abnormalities in conventional markers such as fasting glucose or lipid panels.
For functional practitioners, this creates an important shift in perspective. Erectile dysfunction should not be interpreted simply as a localized reproductive problem. Instead, it can be understood as an early indicator of systemic metabolic stress affecting endothelial signaling, mitochondrial energy production, and nervous system regulation.
If you are training as a functional practitioner or expanding your clinical lens beyond symptom management, learning to interpret erectile dysfunction through metabolic physiology can significantly improve early detection of cardiometabolic risk.
Interestingly, this idea aligns with discussions explored in the iThrive Academy blog “Why Insulin Resistance Begins Years Before Type 2 Diabetes Appears”, where metabolic dysfunction develops silently before clinical diagnosis.
In the same way, erectile dysfunction is rarely the beginning of disease. It is usually the first symptom that becomes visible.
The Vascular Reality of Erectile Function
To understand why erectile dysfunction functions as a cardiometabolic signal, practitioners must first appreciate the physiology of erection itself.
An erection is fundamentally a vascular event. When sexual stimulation occurs, nitric oxide is released from endothelial cells and nerve terminals in penile tissue. This nitric oxide activates cyclic GMP pathways that relax smooth muscle within the penile arteries and corpora cavernosa. As these vessels dilate, blood flow increases dramatically, creating rigidity.
This process depends on several physiological systems functioning in harmony.
The vascular endothelium must produce sufficient nitric oxide. The autonomic nervous system must shift toward parasympathetic dominance. Smooth muscle cells must respond appropriately to signaling molecules. Mitochondria must generate adequate cellular energy to sustain vascular relaxation.
If any part of this signaling network becomes impaired, erectile function can be compromised.
From a cardiometabolic perspective, the key issue is endothelial health. The penile arteries are significantly smaller than coronary arteries. Because of this, endothelial dysfunction appears in penile circulation earlier than in larger vascular beds.
This is why erectile dysfunction frequently appears several years before cardiovascular disease becomes clinically evident.
The penis essentially becomes an early diagnostic window into vascular health.
This concept mirrors ideas discussed in the iThrive Academy blog “Insulin Resistance Is Not Just About Blood Sugar”, which explains how metabolic dysfunction impacts vascular and neurological signaling throughout the body.
Insulin Resistance and the Nitric Oxide Problem
One of the most underappreciated drivers of erectile dysfunction in modern populations is insulin resistance.
Insulin is commonly understood as a hormone responsible for glucose metabolism. However, insulin also plays a critical role in vascular signaling. When insulin binds to its receptor on endothelial cells, it stimulates nitric oxide production through the PI3K signaling pathway.
In metabolically healthy individuals, this pathway helps maintain proper vascular dilation and blood flow.
But in insulin resistant states, this signaling becomes impaired. While insulin levels rise in an attempt to regulate glucose, endothelial nitric oxide production becomes blunted.
The result is a paradoxical situation.
Insulin levels are elevated, yet vascular relaxation becomes increasingly impaired.
This reduction in nitric oxide availability contributes directly to erectile dysfunction by preventing adequate vasodilation in penile arteries.
Over time, chronic hyperinsulinemia also contributes to inflammation, oxidative stress, and further endothelial damage. This creates a metabolic environment where vascular signaling becomes progressively dysfunctional.
For functional practitioners, this means that erectile dysfunction should trigger a deeper investigation into metabolic health markers such as fasting insulin, HOMA IR, triglyceride to HDL ratio, and inflammatory indicators.
The symptom is visible. The root cause is often metabolic.
The Nervous System Connection: Sympathetic Overdrive
While vascular dysfunction is central to erectile physiology, the nervous system plays an equally critical role.
An erection is fundamentally a parasympathetic dominated event. The parasympathetic nervous system promotes relaxation, vasodilation, and reproductive function. In contrast, sympathetic activation favors stress responses and vascular constriction.
In modern lifestyles characterized by chronic stress, sleep disruption, and digital overload, sympathetic nervous system dominance has become increasingly common.
Persistent sympathetic activation increases circulating catecholamines such as adrenaline and noradrenaline. These hormones constrict blood vessels and inhibit the parasympathetic signaling required for erectile function.
This autonomic imbalance can suppress erectile capacity even in men without severe vascular disease.
For practitioners trained in functional medicine, this observation is important. Erectile dysfunction is not always driven purely by testosterone deficiency or vascular obstruction. Sometimes the underlying driver is nervous system dysregulation.
Chronic stress, circadian rhythm disruption, and poor sleep can all impair parasympathetic activity.
Understanding this connection allows practitioners to address lifestyle, stress physiology, and circadian biology as part of a comprehensive therapeutic strategy.

The Nervous System Connection: Sympathetic Overdrive
While vascular dysfunction is central to erectile physiology, the nervous system plays an equally critical role.
An erection is fundamentally a parasympathetic dominated event. The parasympathetic nervous system promotes relaxation, vasodilation, and reproductive function. In contrast, sympathetic activation favors stress responses and vascular constriction.
In modern lifestyles characterized by chronic stress, sleep disruption, and digital overload, sympathetic nervous system dominance has become increasingly common.
Persistent sympathetic activation increases circulating catecholamines such as adrenaline and noradrenaline. These hormones constrict blood vessels and inhibit the parasympathetic signaling required for erectile function.
This autonomic imbalance can suppress erectile capacity even in men without severe vascular disease.
For practitioners trained in functional medicine, this observation is important. Erectile dysfunction is not always driven purely by testosterone deficiency or vascular obstruction. Sometimes the underlying driver is nervous system dysregulation.
Chronic stress, circadian rhythm disruption, and poor sleep can all impair parasympathetic activity.
Understanding this connection allows practitioners to address lifestyle, stress physiology, and circadian biology as part of a comprehensive therapeutic strategy.
Why Erectile Dysfunction Matters for Early Disease Detection
One of the most valuable lessons for practitioners is that symptoms often appear in the most sensitive tissues first.
Penile arteries are particularly vulnerable to early endothelial damage because of their small diameter and high dependence on nitric oxide mediated signaling.
As a result, erectile dysfunction can appear years before cardiovascular disease becomes clinically evident.
For functional practitioners, this presents a powerful opportunity.
Instead of waiting for overt cardiometabolic disease to develop, early symptoms like erectile dysfunction can prompt deeper investigation into metabolic physiology.
By assessing insulin resistance, inflammatory markers, mitochondrial health, nervous system balance, and lifestyle factors, practitioners can intervene long before irreversible disease develops.
This early detection model represents one of the defining advantages of functional nutrition and systems based healthcare.
For learners entering the field through iThrive Academy, developing this pattern recognition skill is one of the most valuable clinical competencies.
Key Takeaway
Erectile dysfunction should never be interpreted solely as a reproductive or hormonal problem. For functional practitioners, it represents an early cardiometabolic signal that reflects deeper disturbances in endothelial health, insulin signaling, mitochondrial function, and nervous system balance. Because penile arteries are particularly sensitive to vascular dysfunction, symptoms often appear years before cardiovascular disease becomes clinically detectable. By viewing erectile dysfunction through a systems biology lens, practitioners gain the ability to identify metabolic dysfunction at a much earlier stage. This shift from symptom based thinking to root cause analysis allows functional nutrition practitioners to intervene earlier, address underlying metabolic stress, and ultimately improve long term cardiometabolic outcomes for their patients.









.jpg)











