Introduction
If you work with patients dealing with infertility, irregular cycles, low testosterone, erectile dysfunction, or unexplained reproductive symptoms, you have likely noticed a frustrating clinical pattern. Many individuals show clear reproductive dysfunction despite normal looking hormone reports. Estradiol may be within range. Testosterone may appear borderline but not dramatically low. Thyroid numbers may not appear alarming. Yet symptoms persist.
Patients experience fatigue, weight gain, low libido, menstrual irregularities, poor sperm parameters, or erectile difficulties. Conventional frameworks often respond by adjusting hormone levels or recommending symptomatic treatments. However, many practitioners soon discover that hormone replacement alone does not always restore normal reproductive physiology. This is where a systems perspective becomes clinically essential.
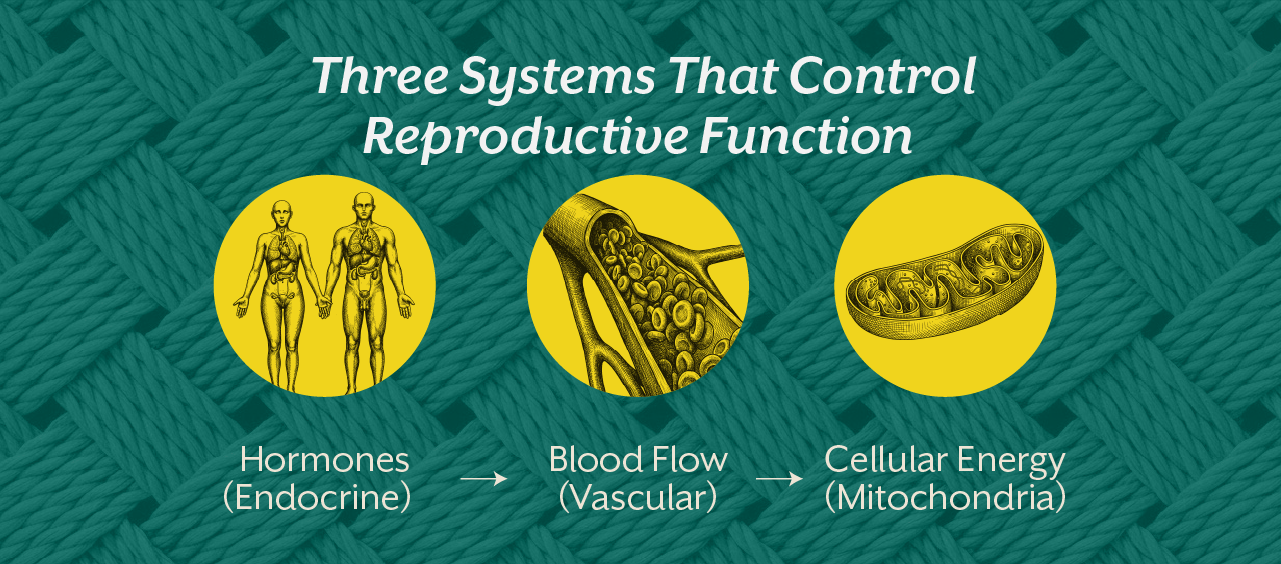
Reproductive physiology is not controlled by hormones alone. It depends on a coordinated interaction between endocrine signaling, vascular function, mitochondrial energy production, and nervous system regulation. When these systems lose synchrony, reproductive dysfunction emerges as a downstream expression of broader metabolic imbalance.
For functional practitioners, understanding this system's model is one of the most important clinical upgrades in reproductive health management.
Interestingly, this system's thinking is very similar to the principles discussed in the iThrive Academy blog “Hypertension Drugs Classification: How BP Medicines Actually Work.” In that article we explored how vascular regulation is not governed by a single pathway but by a network of interacting mechanisms.
Reproductive physiology operates through a similar principle.
You are not treating a reproductive organ in isolation. You are working with an integrated physiological network.
The Endocrine Axis Is Only the Beginning
Most reproductive education begins with the hypothalamic pituitary gonadal axis.
- GnRH is released from the hypothalamus.
- LH and FSH are secreted from the pituitary.
- Sex hormones are produced by the gonads.
This hormonal cascade is fundamental. However, it is only the signaling layer of reproductive physiology. Hormones act as instructions, but biological instructions require responsive tissues to execute them. For example, testosterone may circulate in the bloodstream, but its biological effects depend on androgen receptor sensitivity, mitochondrial energy availability, and adequate vascular delivery. Similarly, ovarian follicles require not only hormonal stimulation but also adequate mitochondrial function to support oocyte maturation.
In clinical practice, many patients present with reproductive symptoms even when hormone levels appear adequate. This disconnect occurs because endocrine signals are only one piece of the system. Without cellular energy, vascular responsiveness, and metabolic stability, endocrine signals cannot translate into physiological outcomes.
Understanding this gap between hormone presence and hormone effect is a crucial step in improving reproductive outcomes.
Mitochondria and Reproductive Energy Demands
Reproductive tissues have some of the highest energy demands in human physiology. Oocyte maturation, sperm motility, hormone synthesis, and tissue remodeling all require substantial ATP production. Mitochondria play a central role in this process.
Oocytes contain thousands of mitochondria because early embryonic development depends heavily on maternal mitochondrial energy stores. Similarly, sperm motility depends on efficient mitochondrial energy production in the midpiece of the sperm cell.
When mitochondrial efficiency declines, reproductive performance often declines as well. In conditions such as insulin resistance, metabolic syndrome, and chronic inflammation, mitochondrial function is frequently impaired.
ATP production becomes inefficient. Oxidative stress increases. Cellular signaling becomes unstable. Over time, this metabolic environment affects reproductive tissues.
Follicular development may slow. Sperm motility may decline. Hormone synthesis may become irregular.
For practitioners, this is why reproductive symptoms often appear alongside metabolic conditions such as obesity, insulin resistance, and chronic fatigue.
Vascular Function and Reproductive Blood Flow
Reproductive organs are extremely dependent on microvascular circulation.
Ovarian follicles require consistent nutrient and oxygen delivery during maturation. Testicular tissue requires stable circulation to support spermatogenesis. Erectile function depends on highly responsive vascular dilation.
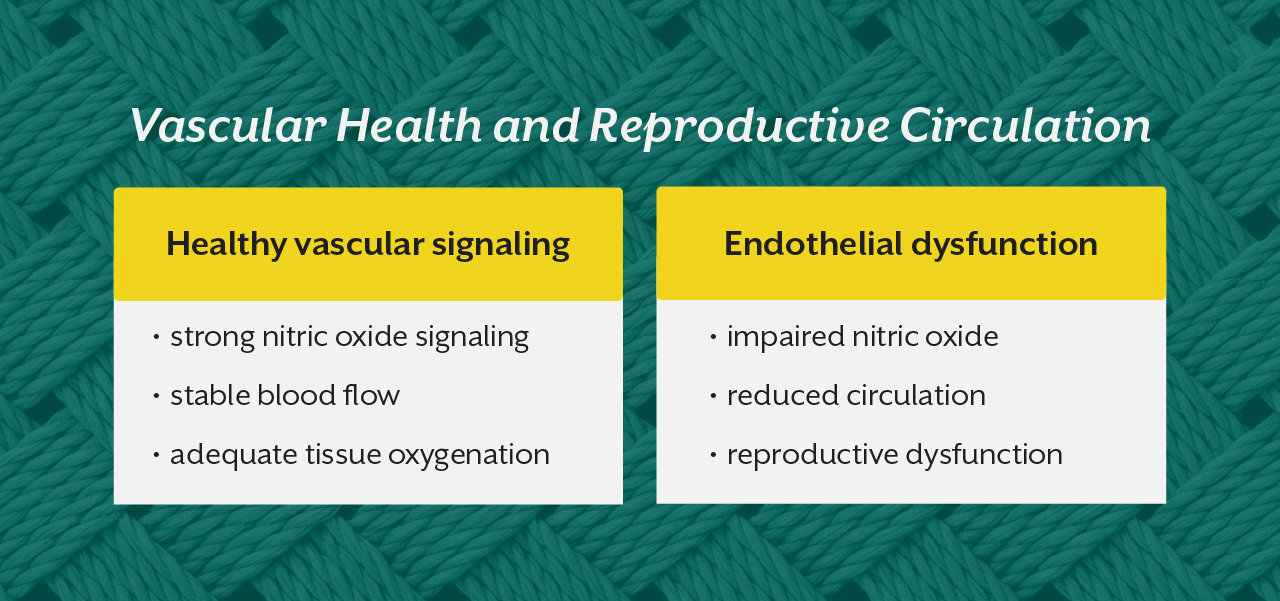
Endothelial health therefore becomes a major determinant of reproductive function.
Nitric oxide is one of the most important signaling molecules regulating vascular relaxation. When endothelial function is impaired, nitric oxide signaling becomes weaker and vascular responsiveness declines. This process is commonly observed in cardiometabolic disorders.
Patients with insulin resistance, hypertension, or chronic inflammation frequently show reduced endothelial function. As vascular health declines, reproductive tissues become more vulnerable to dysfunction. This is one reason why erectile dysfunction is often an early marker of cardiovascular disease.
From a clinical perspective, reproductive symptoms can therefore act as an early warning signal for broader cardiometabolic risk.
The Nervous System and Reproductive Signaling
Reproductive physiology is also tightly regulated by the autonomic nervous system.
Parasympathetic activity supports sexual arousal, erectile function, and reproductive relaxation responses. Sympathetic activation, on the other hand, can inhibit reproductive signaling during periods of stress.
Chronic sympathetic dominance, which is common in modern lifestyles, can therefore suppress reproductive physiology.
Persistent stress signals alter hormone pulsatility, reduce vascular responsiveness, and impair metabolic regulation.
For practitioners, this means reproductive dysfunction cannot be assessed purely through laboratory reports.
Lifestyle stress, sleep quality, nervous system tone, and metabolic health all influence reproductive signaling.
In functional medicine education, this broader systems approach is increasingly emphasized.
Students in the iThrive Certified Functional Nutrition program often explore how metabolic health, nervous system regulation, and endocrine signaling interact across multiple physiological systems.
This integrative understanding helps practitioners move beyond symptom management toward root cause identification.
A Systems Model for Clinical Practice
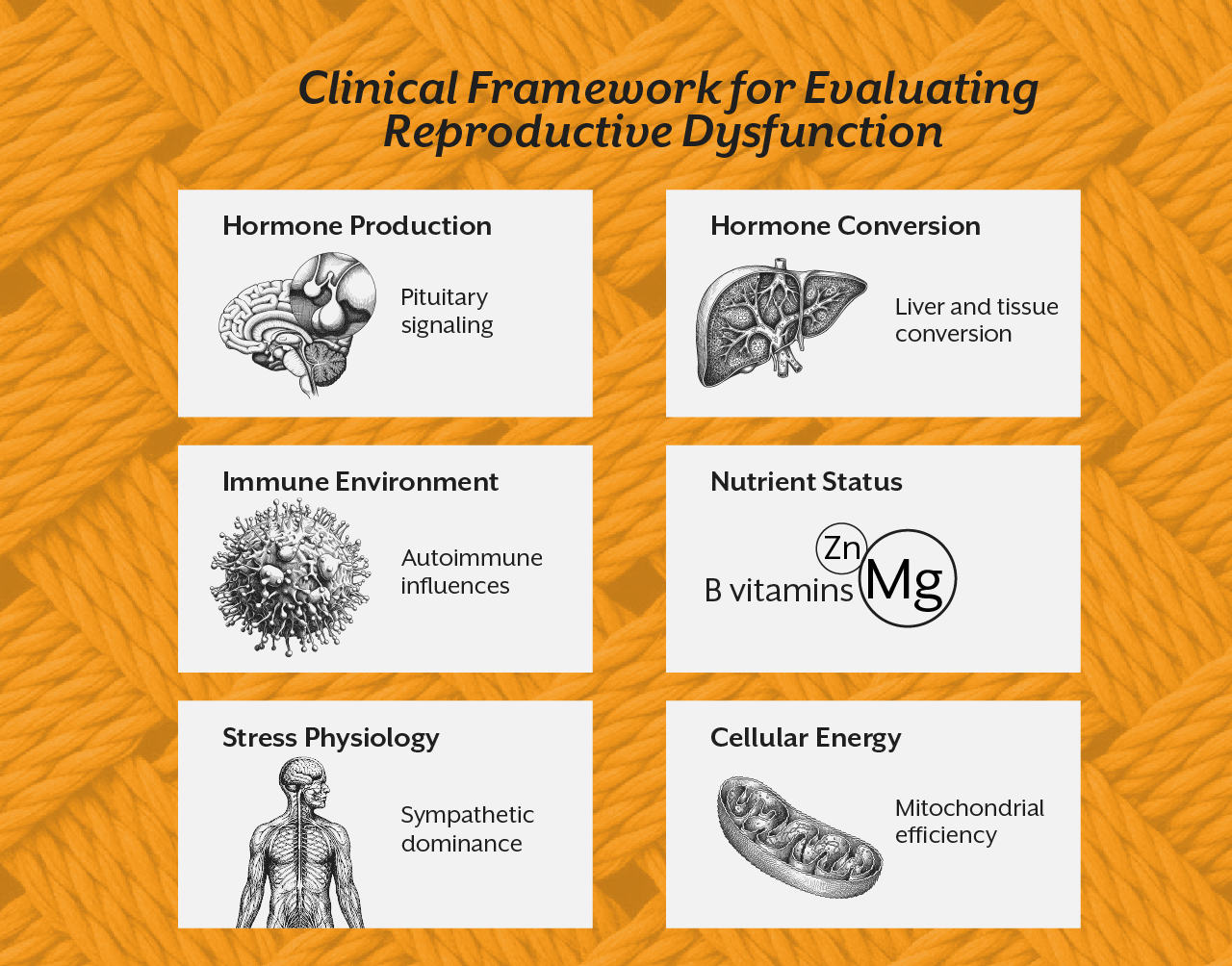
When reproductive dysfunction is approached through a systems perspective, the clinical framework becomes more comprehensive.
Instead of focusing exclusively on hormone levels, practitioners evaluate multiple physiological domains.
- Endocrine signaling provides hormonal instructions.
- Mitochondria provide cellular energy.
- The vascular system delivers nutrients and oxygen.
- The nervous system coordinates physiological responses.
When these systems function harmoniously, reproductive physiology operates efficiently.
When one or more systems become impaired, reproductive symptoms may emerge long before overt disease develops.
For functional practitioners, reproductive health therefore becomes a window into broader metabolic regulation.
Patients presenting with fertility challenges, hormonal imbalance, or sexual dysfunction often provide valuable clinical insights into underlying metabolic and cardiovascular health.
Understanding these patterns allows practitioners to intervene earlier and more effectively.
Key Takeaway
Reproductive dysfunction should not be viewed as an isolated hormonal problem. It is often the visible expression of deeper systemic imbalances involving endocrine signaling, vascular health, mitochondrial energy production, and nervous system regulation. When these systems fall out of alignment, reproductive tissues become vulnerable to dysfunction even when hormone levels appear normal. For functional practitioners, adopting a systems based clinical framework transforms how reproductive symptoms are interpreted. Instead of chasing isolated hormone numbers, the focus shifts toward restoring metabolic resilience, vascular function, cellular energy production, and nervous system balance. This integrative perspective ultimately leads to more meaningful and sustainable clinical outcomes.










.jpg)











