Introduction
If you are a practitioner working with chronic disease today, you have probably noticed something interesting. Many patients who present with metabolic conditions such as obesity, hypertension, insulin resistance, or fatigue often report long standing sleep problems. Sometimes it is mild insomnia. Sometimes it is severe daytime sleepiness. And quite often, after deeper investigation, the diagnosis is obstructive sleep apnea.
Conventional management of sleep apnea is dominated by mechanical therapy. Continuous Positive Airway Pressure or CPAP is widely prescribed and can significantly improve symptoms by preventing airway collapse during sleep. However, if you work closely with patients, you will recognize an important pattern. CPAP manages the airway obstruction, but the underlying metabolic terrain that contributed to the disorder frequently remains unaddressed.
For functional nutrition practitioners, this raises an important question.
What if sleep apnea is not only a structural airway problem but also a systemic metabolic condition?
Emerging research suggests that obstructive sleep apnea is deeply interconnected with inflammation, mitochondrial dysfunction, autonomic nervous system imbalance, insulin resistance, and circadian rhythm disruption. In other words, sleep apnea often reflects deeper physiological dysfunction rather than a single mechanical problem.
Understanding this connection is essential for practitioners who want to move beyond symptom management and address the root drivers of disease. In this blog we will explore how functional nutrition offers a broader framework for understanding and managing sleep apnea, and why practitioners today need to integrate metabolic and circadian biology into sleep medicine.
Sleep Apnea Is Not Only an Airway Disorder
Most textbooks describe obstructive sleep apnea as a mechanical issue. During sleep the muscles supporting the upper airway relax, causing intermittent obstruction. These episodes lead to reduced oxygen levels, repeated awakenings, and fragmented sleep.
But the story does not end there.
Each apnea episode creates a cascade of physiological stress. Intermittent hypoxia triggers oxidative stress. Oxygen deprivation followed by reoxygenation generates reactive oxygen species that damage mitochondrial structures and impair cellular respiration.
Simultaneously, the body activates the sympathetic nervous system to restore breathing. This repeated activation keeps the body in a chronic stress response state throughout the night.
Over time this leads to several systemic consequences:
• chronic inflammation
• endothelial dysfunction
• insulin resistance
• hormonal dysregulation
• metabolic inflexibility
These mechanisms explain why sleep apnea frequently coexists with obesity, hypertension, fatty liver disease, and metabolic syndrome.
If you are teaching students or training practitioners, this is an important concept to emphasize. Sleep apnea is rarely an isolated disease. It is often a manifestation of systemic metabolic stress.
For a deeper exploration of how metabolic dysfunction develops long before disease diagnosis, practitioners may find useful insights in the iThrive Academy article “Insulin Resistance: The Hidden Metabolic Trigger Behind Type 2 Diabetes.” Understanding metabolic roots allows practitioners to design interventions that extend beyond airway management.

The Mitochondrial and Metabolic Dimension of Sleep Apnea
When we examine sleep apnea through a functional medicine lens, mitochondria become central to the discussion.
Neurons regulating breathing, circadian rhythms, and sleep architecture require high energy availability. These brain regions rely heavily on mitochondrial ATP production. When mitochondrial efficiency declines, neuronal signaling within sleep regulating centers can become impaired.
Intermittent hypoxia seen in sleep apnea places significant stress on mitochondria. Excessive reactive oxygen species damage mitochondrial DNA and disrupt the electron transport chain. This leads to reduced ATP generation and increased oxidative damage.
From a clinical perspective, mitochondrial dysfunction has several consequences that practitioners frequently observe in patients with sleep disorders:
- Persistent fatigue despite adequate sleep opportunity
- Cognitive fog and poor concentration
- Reduced stress resilience
- Impaired metabolic flexibility
These symptoms are often dismissed as secondary consequences of poor sleep. However, they may actually reflect deeper cellular energy dysfunction.
Functional nutrition interventions that support mitochondrial health therefore become highly relevant. Nutrients such as magnesium, B vitamins, Coenzyme Q10, Marine Omega 3, and antioxidants support mitochondrial respiration and help restore cellular energy metabolism.
For learners pursuing deeper expertise in these mechanisms, the iThrive Certified Functional Nutritionist (iCFN) program explores mitochondrial biology and metabolic regulation in clinical practice.
Understanding mitochondrial physiology can fundamentally change how practitioners approach chronic disease management.
The Nervous System Factor Most Practitioners Miss
Another dimension of sleep apnea that deserves greater attention is autonomic nervous system imbalance.
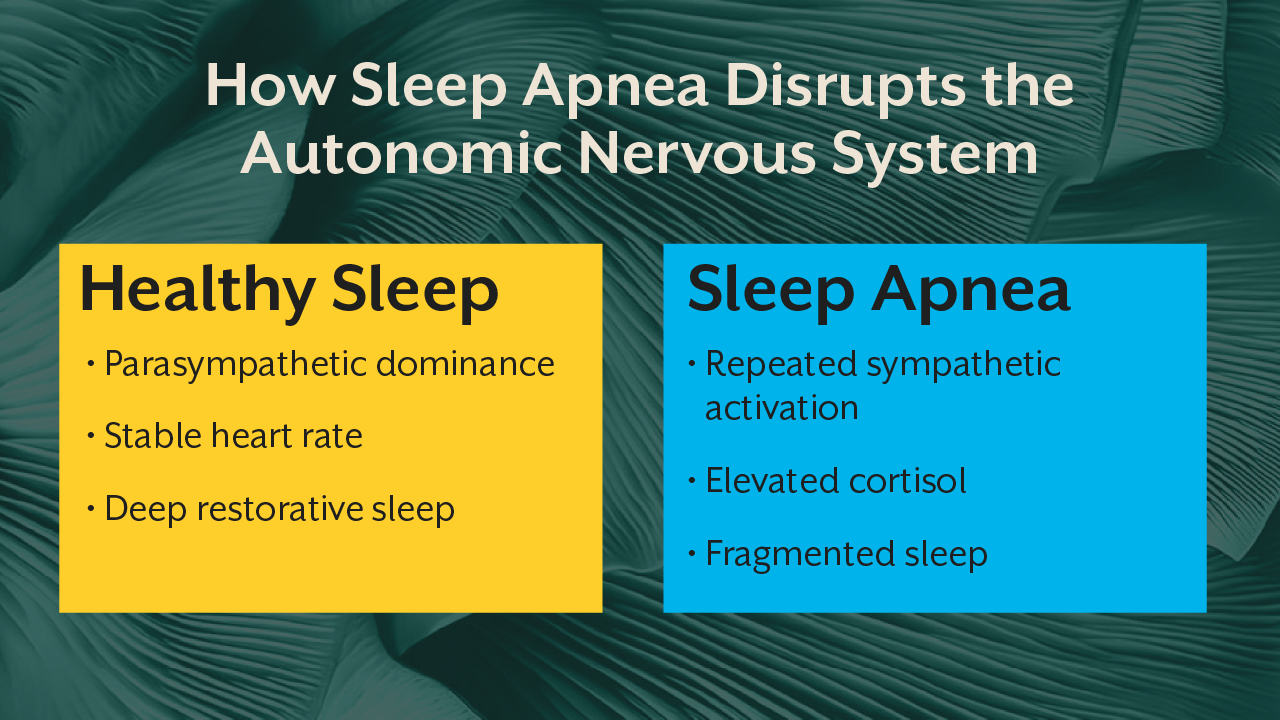
During normal sleep, the parasympathetic nervous system dominates. This allows physiological recovery, hormonal regulation, and cellular repair. In individuals with sleep apnea, however, repeated breathing disruptions trigger sympathetic activation.
Every apnea episode acts like a micro stress event. The brain senses oxygen deprivation and immediately activates survival responses. Heart rate increases, cortisol rises, and the body shifts into a fight or flight state.
Imagine this occurring dozens or even hundreds of times each night.
Over time this leads to chronic autonomic dysregulation. Patients may experience elevated blood pressure, poor stress tolerance, increased anxiety, and difficulty transitioning into deep restorative sleep. This explains why simply correcting airway obstruction does not always resolve all symptoms. The nervous system may remain dysregulated even after CPAP therapy begins.
Functional approaches that support autonomic balance therefore become critical. These include circadian rhythm alignment, stress management techniques, breathwork practices, and physical activity that enhances vagal tone. These interventions help restore parasympathetic dominance and improve sleep architecture.
Why Metabolic Health Determines Sleep Quality
If you examine clinical data across populations, one pattern becomes clear. Sleep apnea prevalence increases significantly in individuals with metabolic dysfunction.
Obesity contributes to airway narrowing due to adipose tissue deposition around the neck and pharyngeal structures. But metabolic dysfunction goes deeper than structural changes.
Insulin resistance alters hormonal signaling involving leptin and ghrelin. These hormones regulate appetite, metabolism, and energy balance. When their signaling becomes disrupted, patients may experience increased hunger, weight gain, and further metabolic stress. Sleep deprivation itself worsens insulin sensitivity. In other words, sleep apnea and metabolic dysfunction reinforce each other in a vicious cycle. Breaking this cycle requires metabolic rehabilitation rather than symptom suppression alone.
This is where functional nutrition strategies become particularly valuable. Dietary patterns emphasizing whole foods, anti-inflammatory nutrients, and stable glycemic regulation can reduce systemic inflammation and improve metabolic flexibility.
Practitioners who already work with metabolic disorders will recognize similar mechanisms discussed in the iThrive Academy article “Metabolic Syndrome Explained: The Hidden Drivers of Chronic Disease.” Sleep health and metabolic health are deeply interconnected physiological systems.
Functional Nutrition Strategies That Complement CPAP
Functional nutrition does not replace conventional treatment for sleep apnea. Mechanical therapies such as CPAP remain important for preventing airway collapse and restoring oxygenation. However, addressing the metabolic terrain significantly improves long term outcomes.
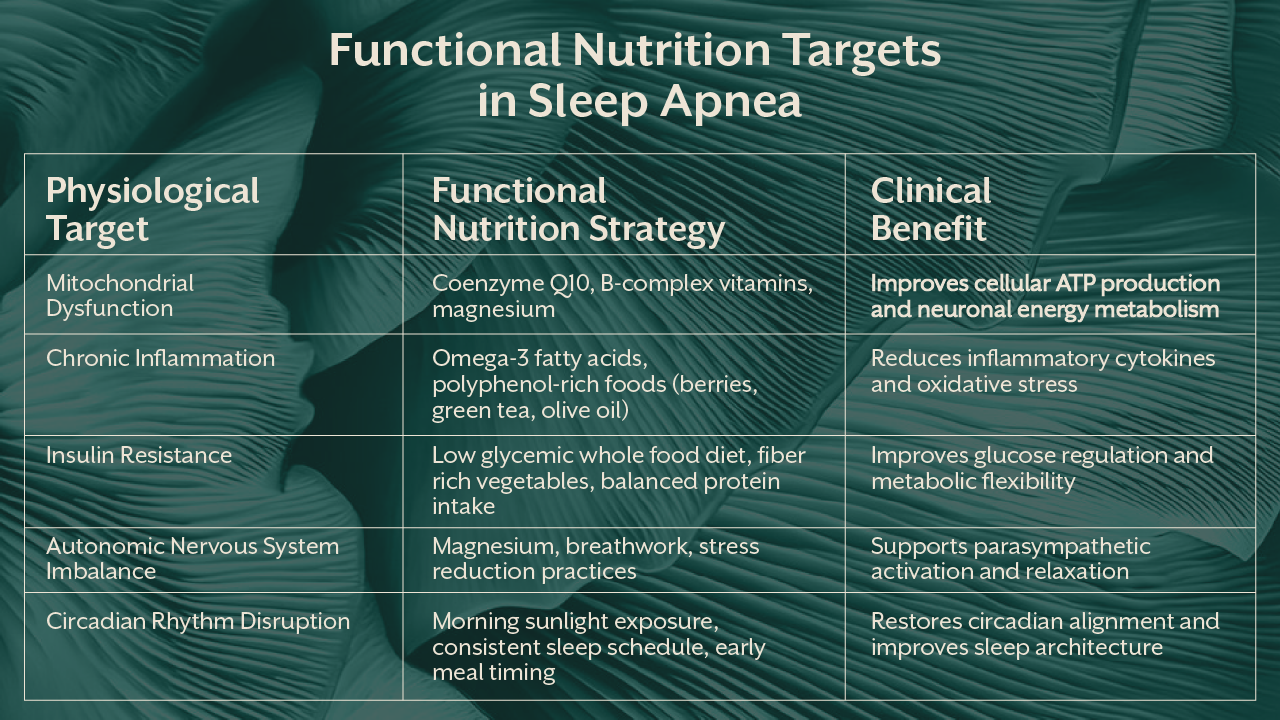
Dietary interventions aimed at reducing systemic inflammation are particularly valuable. Whole food dietary patterns rich in vegetables, healthy fats, and phytonutrients help reduce oxidative stress and support mitochondrial function.
Targeted micronutrients also play a key role. Magnesium supports neuromuscular relaxation and nervous system balance. B vitamins contribute to mitochondrial energy metabolism. Omega 3 fatty acids reduce inflammatory signaling pathways. Coenzyme Q10 improves mitochondrial electron transport efficiency.
Circadian alignment strategies are equally important. Consistent sleep timing, reduced evening blue light exposure, and daytime sunlight exposure help synchronize the central circadian clock located in the suprachiasmatic nucleus. When these metabolic and circadian factors are optimized, practitioners often observe improvements in energy levels, metabolic markers, and overall sleep quality.
Why Practitioners Must Learn an Integrative Sleep Framework
If you are educating future practitioners or expanding your own clinical knowledge, sleep medicine represents one of the most interdisciplinary fields in healthcare. It intersects with metabolic health, neurology, endocrinology, nutrition science, and circadian biology. Unfortunately, traditional medical training often examines these systems separately.
Functional nutrition training attempts to bridge these gaps by teaching practitioners how physiological systems interact. Programs such as the iThrive Certified Functional Nutrition (iCFN) course are designed to help practitioners understand these connections in real clinical scenarios. Instead of viewing diseases in isolation, students learn to evaluate metabolic pathways, inflammatory markers, lifestyle factors, and dietary patterns together.
For practitioners seeking to expand their clinical toolkit, this integrative perspective is becoming increasingly important.
Key Takeaway
Obstructive sleep apnea is far more complex than a simple airway disorder. While CPAP therapy effectively addresses the mechanical obstruction that characterizes the condition, the underlying physiological terrain often involves chronic inflammation, mitochondrial dysfunction, metabolic dysregulation, and autonomic nervous system imbalance. Functional nutrition offers practitioners a broader lens through which to understand these interactions. By addressing metabolic health, supporting mitochondrial function, restoring circadian alignment, and improving nervous system regulation, practitioners can complement conventional treatments and help patients achieve more sustainable improvements in sleep quality and overall health. For clinicians, educators, and learners alike, integrating sleep physiology with metabolic and nutritional science represents an important step toward more comprehensive and effective healthcare.










.jpg)











